THE MOST POWERFUL & BENEFICIAL CBD PRODUCTS AVAILABLE

- Bullet 1
- Bullet 2
- Bullet 3
THE MOST POWERFUL & BENEFICIAL CBD PRODUCTS AVAILABLE
Experience the CBDPure Difference
Contains all-natural Cannabidiol (CBD), Terpenes, and
other Cannabinoids

Guaranteed
Your satisfaction is our top priority, which is why your order is backed by our 90 Day Money-Back Guarantee.

Organic Standards
Our CBD oil is made with hemp grown using organic-standards in Colorado and Washington, free of contaminants and additives.

Quality Tested
All products are quality tested by an independent third-party lab to ensure you get the best product possible, and the potency results are made public for your review.

Satisfaction
Join our thousands of satisfied CBD customers from all walks of life and find out first-hand the difference CBDPure can make, satisfaction guaranteed.

What is CBD?
CBD (Cannabidiol) is a potent, non-psychoactive cannabinoid derived from hemp. It is typically extracted from hemp plants that are naturally high in CBD and other phytonutrients. It is the most prevalent of over 80 different cannabinoids found in hemp.
Shop CBDPure



The Science Behind CBDPure
Cold Pressed Hemp Seed Oil
CBDPure uses cold-press hemp seed oil as the carrier matrix because its flavor profile complements the full-spectrum oil. It is also packed with healthy omega-3 and omega-6 fatty acids, is virtually flavorless and is shelf-stable.
CO2 Extracted CBD Oil
We choose to use CO2-extracted CBD oil in our products because it is a highly effective and safe method for extracting full-spectrum CBD oil. This method helps to ensure that the oil we produce is pure, clean, and safe for use.
Full-Spectrum Cannabinoids
CBDPure contains a full range of cannabinoids and phytonutrients, as compared to CBD isolate alone.
Organically Grown Hemp
CBDPure never compromises on quality and only contains the purest CBD oil from hemp grown using organic standards from Colorado and Washington.
Sublingual Oral Delivery
CBDPure CBD oils are taken under the tongue and quickly absorbed for faster health benefits.
The Magic Behind
Full-Spectrum Oil
Full-spectrum CBD oil contains all the beneficial phytonutrients found in hemp plants. These include a wide variety of cannabinoids, such as CBD and trace amounts of THC, terpenes and flavonoids.
When all these phytonutrients are consumed within a full-spectrum oil, they have a synergistic effect on the endocannabinoid system. The effect is often referred to as the “Entourage Effect”.
The Entourage Effect is the body's reaction to the combination of cannabinoids, terpenes and flavonoids. Scientists have not quite figured out why this happens, but they have observed that this effect is less present when phytonutrients are consumed in their isolated form.
You Deserve the Best CBD.

Organic Excellence: The Heart of CBDPure Products
Discover the purest form of wellness with CBDPure's USDA Certified Organic offerings, including CBDPure 300, 600, 1000, and CBDPet. Each product in this select range adheres to rigorous organic standards, offering you a trusted source of high-quality, naturally potent CBD to support your health and well-being.
In addition to our USDA Certified Organic products, we maintain the same exacting standards across our entire product line. This commitment extends to CBDPure Softgels, Muscle and Joint Cream, Relief, Calm, and Sleep, all crafted with the same USDA Certified Organic CBD oil. Our unwavering dedication to quality ensures that every CBDPure product delivers the utmost in organic purity and effectiveness.
CBDPure is more than just a range of CBD products; it's a commitment to natural, safe, and effective wellness solutions. Embrace the CBDPure difference, where the finest natural elements meet our stringent quality standards, setting a new benchmark in CBD excellence and trust.
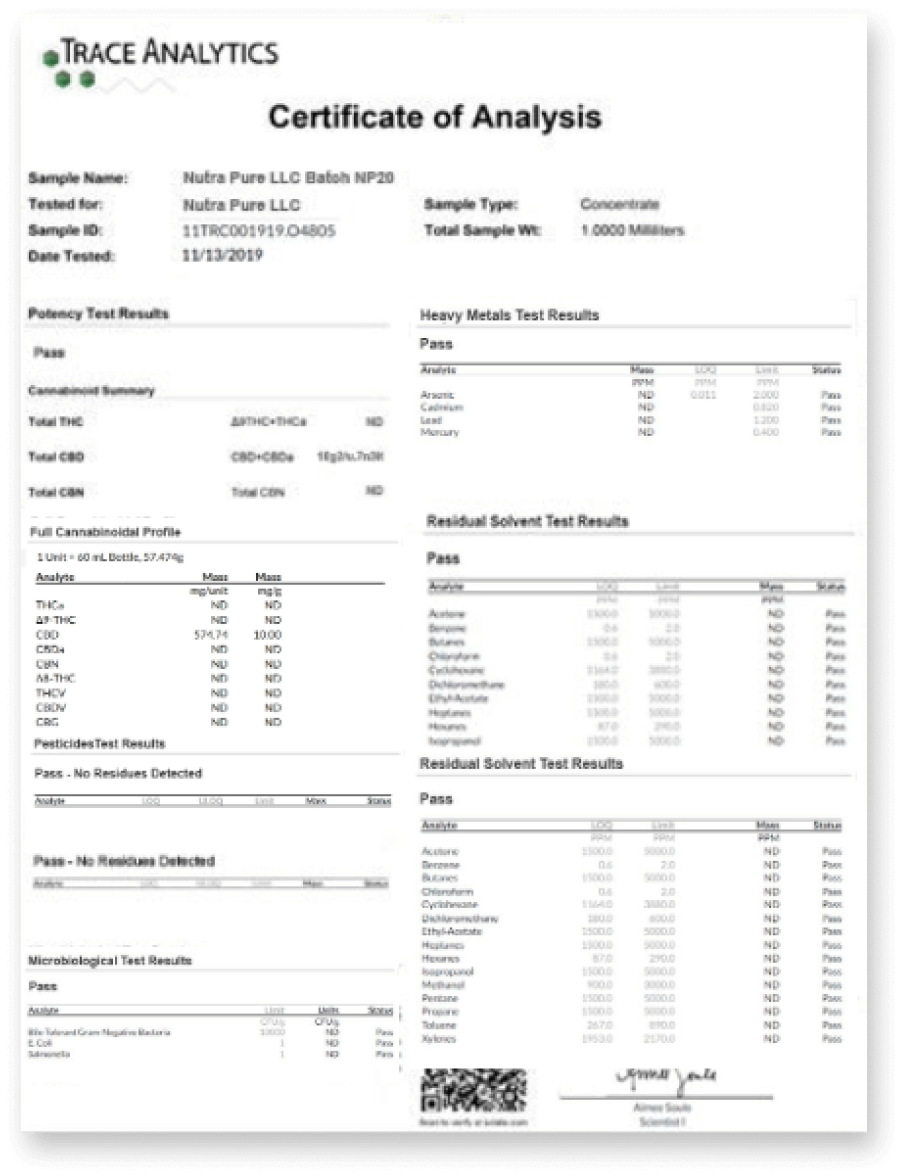
Third-Party Testing
Our CBD oil is third-party tested for potency and quality, and we make public the results of every single test to our clients. Our stringent independent lab-testing program ensures that you get the very best, and most potent, CBD oil available.
Cannabinoid Profiling
Reveals the concentration of active cannabinoids for accurate dosage and to ensure the quality of the product.
Pesticide
Testing
Detects even trace amounts of chemical pesticides in hemp concentrates using advanced testing procedures.
Heavy Metal Testing
Detects trace amounts of heavy metals to ensure the safest product possible.
Microbiological Screening
Determines if there are any microorganisms and harmful pathogens such as bacteria and fungi present in the CBD oil.
Residual Solvent Testing
Identifies and measures harmful solvents, impurities or other foreign chemicals that should not be present after the CBD extraction process.
Shop CBDPure




Need help?
FDA DISCLOSURE
Representations regarding the efficacy and safety of CBDPure have not been evaluated by the Food and Drug Administration. The FDA only evaluates foods and drugs, not supplements like these products. These products are not intended to diagnose, prevent, treat, or cure any disease. Click here and here to find evidence of a test, analysis, research, or study describing the benefits, performance or efficacy of CBD Oil based on the expertise of relevant professionals.
These statements have not been evaluated by the FDA and are not intended to diagnose, treat, or cure any disease. Always check with your physician before starting a new dietary supplement program.
The Cannabidiol (CBD) in CBDPure is a natural constituent of industrial hemp plant and grown in the United States of America. CBDPure does not sell or distribute any products that are in violation of the United States Controlled Substances Act (US CSA).
Thanks for signing up. Here is your coupon: 10PERCENT
Thanks for signing up. Here is your coupon: 10PERCENT
